Each case in the article is followed by few questions about the descriptions of the finding(s) in the CT scan, the differential diagnoses or the diagnosis of the case condition, and about the conditions themselves. The questions are answered briefly in the answers and discussions part to give the reader a simple idea about the findings and diseases.
We tried to vary the case we chose to include in the article to cover the widest possible range of conditions and regions. You will be able to find non-contrast-enhanced CT and contrast-enhanced CT scans of many regions like the brain, paranasal sinuses, temporal bone, chest.
1. Acute limbs weakness and inability to speak
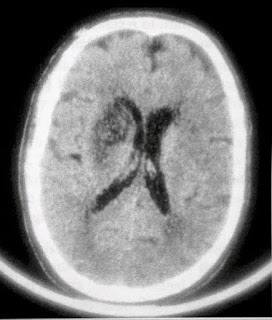
A 69-year-old male with acute weakness of the left side of his face, his left arm, and left leg was brought to the hospital. His initial CT scan was normal. The image below is taken from a head CT scan that he had 3 days later.
Questions
1. What is the finding seen in this scan?
2. What is the diagnosis?
Answers and Discussions
The image shows a hypodense lesion in the territory of the left middle cerebral artery at the region of the right basal ganglia and internal capsule. The lesion has a mass effect in the form of mild compression of the right lateral ventricle. These findings are consistent with acute infarction in the Lenticulostriate arteries on the right side.
The Middle cerebral artery is a branch of the internal carotid artery, and it has four parts (M1, M2, M3 & M4). M1 is called the sphenoidal branch and it is the segment that extends from the origin of the artery to its bifurcation. This segment has four branches; some of them (lateral lenticulostriate arteries) supply the putamen, external capsule, and a part of the internal capsule. The remaining part of the blood supply of the basal ganglia and internal capsule comes from the anterior cerebral artery branches. Medial lenticulostriate arteries, which arise from A 1 segment of the anterior cerebral artery, supply the caudate nucleus and the anterior limb of the internal capsule. The recurrent artery of Heubner, a branch of the A2 segment of the anterior cerebral artery, supplies.
Infarcts in the middle cerebral artery territory are common. They usually present with motor symptoms (hemiparesis), sensory symptoms (hemisensory loss), visual symptoms (hemianopia) and the patient may have aphasia.
Ischemic strokes have three main phases and each of these phases dier from the other on CT scan:
- Hyperacute phase (0-6 hours)
- Acute phase (6-24 hours)
- Subacute phase (1-7 days)
In the hyperacute phase, no signs can be seen in a non-contrast-enhanced CT scan apart from the hyperdense middle cerebral artery and obscured lentiform nucleus in some cases of middle cerebral artery occlusion. In general, changes start to appear in the acute stage. These changes include effacement of sulci and loss of grey-white matter differentiation (both of which are caused by edema), in additional to hypodense basal ganglia and insular cortex due to ischemia in some cases of middle cerebral artery occlusion. changes seen in subacute infarcts include hypodense areas, hemorrhagic transformation, and compression of CSF spaces (ventricles, cisterns) with or without midline shift.
2. Acute left side weakness
A 57-year-old male had an acute weakness of his left upper and lower limbs. He is a known case of hypertension on and off treatment. On admission, his blood pressure was 240/120 mm Hg and he had left-sided hemiparesis and sensory loss. The image below is taken from his head CT scan.
Questions
1. What does the CT image show?
2. What is the likely diagnosis?
Answer and discussion
The image shows a hyperdense lesion in the region of the right thalamus. The lesion is surrounded by a hypodense rim and is compressing the right lateral ventricle and is causing a mild shift of the midline to the left side. The most likely diagnosis is intracerebral hemorrhage.
Cerebrovascular accident (CVA) or stroke is a condition in which there is a reduction or complete obstruction of blood flow to a specific area in the brain and that can lead to brain cell death and permanent disability. There are two types of stroke: ischemic and hemorrhagic. Hemorrhagic strokes are less common than ischemic ones and they constitute about 20% of all strokes.
Hemorrhagic strokes can be classified according to the site of bleeding into intracerebral hemorrhagic strokes is high blood pressure. There are some other less common causes such as coagulopathies, thrombolytic therapy, anticoagulant therapy, vasculitis, aneurysms, and arteriovenous malformations.
The presentation of the patient depends on the affected area and can include symptoms like convulsions or headaches. on examination, some of the following signs might be found: hemiparesis, loss of sensation, aphasia, hemianopia, confusion, facial weakness, or apraxia.
The appearance of the hemorrhage on non-contrast-enhanced CT scan of the brain depends on the age of the hemorrhage:
Acute hemorrhage (less than 1 week old):
- Appears as a hyperdense area (density between 50 and 70 HU).
- If the patient has low hemoglobin or bleeding disorder, it might appear as an isodense area.
- Subacute hemorrhage (1-6 weeks old):
Appears as an isodense area.
- Chronic hemorrhage (older than 6 weeks old):
Appears as a hypodense area.
If there is a rebleeding, then the areas of rebleeding will appear as small hyperdense areas inside the hypodense old hemorrhage.
The mortality rate of patients with hemorrhagic strokes is very high. Only 40% of patients live longer than one year after having a hemorrhagic stroke.
3. An Old Female With Loss Of Consciousness
A 79-Year-old female was brought unconscious to the emergency department. A CT scan of the head without contrast was requested to rule out intracranial pathologies. The image below is taken from her head CT scan.
Questions
1. What are the findings seen in the patient CT scan?
2. What is the diagnosis?
3. What are the types of intracranial hemorrhages and what are their most common causes?
Answer and discussion
The images show hyperdense crescent-shaped extra-axial collections in the left frontoparietal region with a shift of the midline to the left side and hyperdense ventricles. These findings are consistent with left-sided subdural hemorrhage in the left frontoparietal region and bilateral intraventricular hemorrhage inside both lateral ventricles.
Intracranial hemorrhages can be classified into:
Intraaxial hemorrhages:
*Intraparenchymal hemorrhage
*Intraventricular hemorrhage
Extra axial hemorrhages:
*Epidural hemorrhage
*Subdural hemorrhage
*Subarachnoid hemorrhage
Classification of intracranial hemorrhage into intra- and ex-triaxial hemorrhage depends on the location of the hemorrhage. Intraaxial hemorrhages are inside the brain while extra-axial hemorrhages are outside the brain. Intraaxial hemorrhages are usually the more dangerous ones.
In this case, we see one type of extra-axial hemorrhage (subdural hemorrhage) and one type of interaxial hemorrhage (intraventricular hemorrhage). Each of these types can occur alone or with other types and intracranial pathologies.
In subdural hemorrhage, blood accumulates between the brain and the dura. It has many causes, the most common of them are; trauma and anticoagulant therapy. Very young people, very old people, and alcoholics are at more risk of having this type of hemorrhage. Subdural hemorrhage can be acute or chronic and can be sudden onset. They can present with loss of consciousness or they can develop slowly and cause headaches, vomiting, confusion, hemiparesis, or convulsions.
The appearance of subdural hemorrhage on CT scan depends on the age of the hemorrhage. At all times, it will appear as a crescent-shaped lesson between the brain and the skull. In the acute phase, it will appear hyperdense. In the subacute phase, it will be isodense and in the chronic phase, it will have a hypodense appearance.
Intraventricular hemorrhage can be primary (involving only the ventricles) or secondary (extending to ventricles from other location). Usual causes of primary intraventricular hemorrhages are trauma, tumors, aneurysms, and AVM in choroid plexus. Secondary intraventricular hemorrhage can be caused by extension of intraparenchymal or subarachnoid hemorrhage to the ventricles. Usually, there are focal neurological signs with primary intraventricular hemorrhage, and the symptoms tend to be general. Symptoms include sudden headache, vomiting, or change in consciousness level. The mortality rate in patients with intraventricular hemorrhage is about 50-80%.
4. Chronic Headache And Vomiting
A 44-year-old female complains of chronic headache that started a few months ago and is associated with early morning vomit-
ing. The images below are taken from her contrast-enhanced CT scan of the head.

Questions
1. What does the CT Image Show?
2. What is the most likely diagnosis?
3. what are the other symptoms that can be caused by this lesson?
Answers and discussion
The CT images show a single well-defined extra-axial infratentorial-
al focal lesion in the left side of the posterior cranial fossa with
intense homogeneous enhancement. The lesion compresses the left
cerebellar hemisphere and causes a shift of the midline to the left side
with compression of the 4ch ventricle. The most likely diagnosis is
a meningioma.
Meningiomas are brain or spinal cord tumors that arise from the
meninges. They are usually benign and they constitute about 20% of
all primary brain tumors. The presentation of meningiomas depends
on its site and size. When they are in the posterior cranial fossa, they can present in many different ways in addition to presenting with headache and vomiting. The most common of these additional presentations are cranial nerve dysfunction, vermian syndrome, ataxia
(truncal or limb), nystagmus, and dysmetria.
Other tumors can arise in the location of this lesion (in the
posterior cranial fossa). These tumors are intraracial tumors and they
constitute about 15-20% of all brain tumors in adults. These tumors
include:
.
- Metastases
- Haemangioblastoma
- Astrocytomas
- Medulloblastomas
.
Cerebellar metastases are the most common type of posterior cranial fossa tumors. The most common sources for these metastases
are lung and breast cancers. Haemangioblastomas are benign tumors
that arise from the central nervous system vessels. They are the most common primary tumors in the cerebellum, and they constitute about
7-10% of the posterior fossa tumors seen in adults. Astrocytomas
and medulloblastomas are rare in adults.
The differentiation between extra and intra axial tumor depends on finding some characteristic that identifies the extra-axial location of the tumor-like:
Having a white dural base
CSF cleft sign
Finding cortical grey matter between the lesson and The White matter.
5. An Adult Male With Convulsions
A 27-year-old man with recurrent convulsions was admitted to the department of medicine. The patient is a known case of small cell lung cancer in his temperature was normal and his white cell count was 8000 the image below is taken from his head CT Scan before and after contrast administration.
Question
1. What are the finding seen in this scan?
2. What is the differential diagnosis for this finding?
3. What is the most likely diagnosis?
Answers and discussion
The CT image shows an ill-defined and hypodense area in the upper part of the left parietal lobe with finger-like projections before the administration of contrast. After contrast administration, to wale-defined, as scheduled hypodense lesion with ring enhancement is seen. The to listen is surrounded by focal edema.
The differential diagnosis of brain listened with ring and hands mint on CT Scan includes:
CNS Infections:
o Brain abscess
o Tuberculoma
o Neurocysticercosis
CNS tumors:
Metastasis
o Glioblastoma multiforme
In HIV positive patients:
o CNS toxoplasmosis
CNS lymphoma
The most likely diagnosis, in this case, is cerebral metastasis from the patient's lung carcinoma. The most common sources of metastasis to the brain are lung tumors, breast tumors, gastrointestinal tumors, and genitourinary tumors. Metastatic tumors represent about a third of the tumors
found in the brain.
Some patients with brain metastasis are asymptomatic, but the
the majority has one or more of the following symptoms: headache, vomiting, convulsions, focal neurological deficit, or ataxia.
Up to 40% of patients with malignancies have brain metastasis
on the time of diagnosis, and that metastasis can be detected using various imaging modalities. The majority of those metastatic are found in the cerebrum (about 80%). all through brain matter studies are through to be used multiple, studies show that about half of the patients with brain metastasis have solitary Metastasis.





Post a Comment